Therapy
Lower Extremity Tendinopathy
With support of recent studies, rehab specialists are swapping passive treatments (like stretching) for more active and decompressive interventions.
With support of recent studies, rehab specialists are swapping passive treatments (like stretching) for more active and decompressive interventions.
Are you experiencing any of the following: Bladder leakage when you cough, sneeze, laugh, walk or run? Frequent urination so you can’t leave the house or join friends for lunch? Are you getting up 2 more more times at night to urinate? Can’t make it to the bathroom in time? Have to urinate when you hear running water or do dishes? Experience a heavy feeling in your pelvis or like something is falling out? Not Read more…
Squatting Do’s and Dont’s Posted on May 31, 2013 by Kasey Aiken We get asked quite frequently “Is it bad to do squats for a work out?” “How can I protect my spine during work outs?” “It hurts my low back when I’m squatting, do I need to quit?” After observing the squat position of many of our patients, I would prefer to say they should not be squatting until we fix x, y, Read more…
Osteoarthritis is a degenerative joint disease that affects more than 27 million Americans and is the primary cause of long-term disability (Lawrence, et al and Walker, Helena). The risk of developing lower-body osteoarthritis (OA) – for example, in the hip and/or knee joints – is 4 times higher for persons that are obese in comparison to those that maintain a more optimal body weight. Both osteoarthritis and obesity are recognized as global public health problems. Read more…
We get asked a lot to explain what Postural Restoration is in simple terms. Indeed, the concepts are not simple – and in most healthcare providers’ opinions, the ideas are a bit peculiar.
The basis of Postural Restoration lies in an understanding of our anatomy and an appreciation that our bodies are not symmetrical and never will be. The fact that we have one of some organs (ie: heart and liver), as well as organs that are shaped differently on one side of our body compared to the other (ie: lungs and diaphragm), results in mild asymmetrical positioning of our bones and muscles. Consequently, movement of our limbs, trunk, and spine tends to be easier or harder on one side in comparison to the other. A good look in the mirror will reveal mild to drastic differences in the appearance of our rib cage, shoulder height, foot position, and even ears or eyes, when comparing right versus left.
Scoliosis is a diagnosis that makes people think of many undesireable things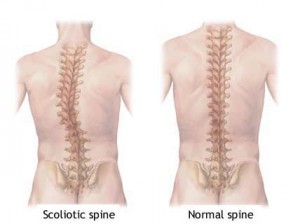 – back pain, bracing, surgery, disfiguration. What people may not realize is that often a diagnosis of scoliosis leads to a course of orthopedic physical therapy. S.T.A.R. PT has been practicing a somewhat unique approach to conservatively treating scoliosis. We understand that we will not be able to completely correct the spinal curvature in idiopathic scoliosis, but we believe that much can be gained from a program to manage the curvature by reducing musculoskeletal torsion and improving the mechanics of the thorax.
– back pain, bracing, surgery, disfiguration. What people may not realize is that often a diagnosis of scoliosis leads to a course of orthopedic physical therapy. S.T.A.R. PT has been practicing a somewhat unique approach to conservatively treating scoliosis. We understand that we will not be able to completely correct the spinal curvature in idiopathic scoliosis, but we believe that much can be gained from a program to manage the curvature by reducing musculoskeletal torsion and improving the mechanics of the thorax.
Many patients at S.T.A.R. PT will find themselves squatting – for evaluative purposes or as a part of their treatment program. Squatting is one of the most typical ‘functional movement patterns’ that persons of all ages and physical ability levels are required to do during a multitude of daily tasks. Therefore, it is important to be able to successfully complete this activity.